Understanding the Connection Between Them and Treatment Options
Obstructive Sleep Apnea (OSA) and Restless Leg Syndrome (RLS) are two common sleep disorders that often coexist in patients, leading to correlated sleep disturbances and health issues. While sleep disorders often times overlap, it's essential to explore the specific relationship between OSA and RLS.
"Recognizing and treating the overlap between obstructive sleep apnea and restless leg syndrome is crucial. Addressing these two conditions can lead to improved overall sleep health and quality of life," says Robert Miller, Apria's Vice President of Sleep Business.
What is Obstructive Sleep Apnea (OSA)?
OSA is a prevalent sleep disorder characterized by multiple episodes of partial or complete blockage of the airway during sleep. These blockages lead to breathing pauses, resulting in frequent awakenings throughout the night. Common symptoms of OSA include loud snoring, gasping for air during sleep, and excessive daytime sleepiness. OSA not only disrupts sleep but also poses health risks, such as heart disease, stroke, diabetes, and high blood pressure.
What is Restless Leg Syndrome (RLS)?
RLS is another sleep disorder marked by an irresistible urge to move the legs that is typically considered to be very uncomfortable. These symptoms usually occur in the evening or at night, making it difficult for individuals to fall asleep. The exact cause of RLS remains unknown, but it is often associated with various underlying conditions.
Risk Factors for RLS
RLS shares some risk factors with OSA, though there are obvious differences. RLS tends to be more prevalent in women and increases with age. Key risk factors include:
- Peripheral Neuropathy: Damage to the nerves in the hands and feet, often due to chronic conditions like diabetes or alcohol use disorder.
- Iron Deficiency: Low iron levels, common in individuals with anemia, gastrointestinal bleeding, heavy menstrual periods, or frequent blood donors.
- Kidney Failure: Kidney dysfunction can lead to iron deficiency and anemia, enhancing RLS symptoms.
- Spinal Cord Conditions: Injuries or conditions affecting the spinal cord.
- Parkinson's Disease: Certain medications for Parkinson's disease, particularly dopaminergic agonists, can increase the risk of RLS.
Certain medications, such as antidepressants, anti-nausea drugs, antihistamines, and even sleep deprivation, can have an effect on RLS symptoms.
Diagnosing RLS
Diagnosing RLS requires a comprehensive evaluation by a healthcare professional. Blood tests are often conducted to check for low iron levels. Patients may be referred to a sleep specialist for a sleep study. The diagnosis is based on criteria established by the International Restless Legs Syndrome Study Group, which includes:
- An irresistible urge to move the legs, usually with uncomfortable sensations.
- Symptoms that start or worsen during periods of rest or inactivity.
- Partial or temporary relief of symptoms through activity, such as walking or stretching.
- Symptoms that worsen in the evening or nighttime.
- Symptoms that cannot be attributed solely to another condition.
Treating RLS
Treatment for RLS often focuses on addressing any underlying conditions, such as iron deficiency. When no underlying cause is found, lifestyle changes like maintaining good sleep habits are recommended. In some cases, medications such as muscle relaxants or drugs that increase dopamine levels in the brain may be prescribed.
The Relationship Between OSA and RLS
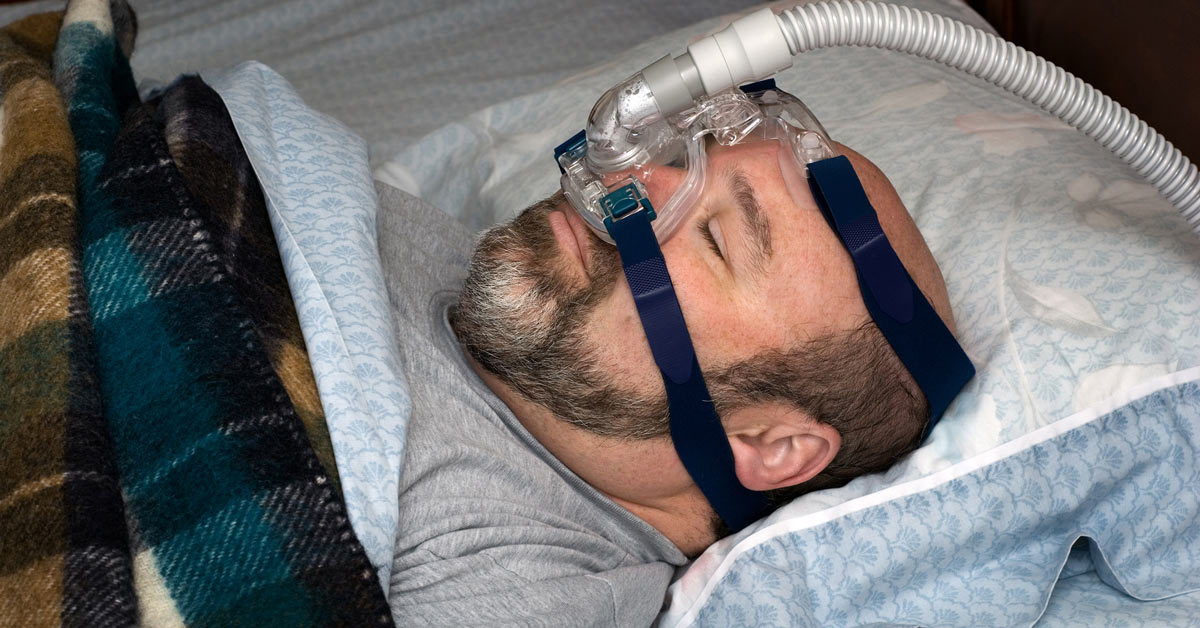
While OSA and RLS commonly coexist, they do not share a known underlying cause. The primary connection between the two is their prevalence in the general population. However, untreated sleep apnea can lead to sleep deprivation, a known trigger for worsening RLS symptoms. This overlap highlights the importance of proper diagnosis and treatment. For instance, patients using Continuous Positive Airway Pressure (CPAP) therapy for OSA should continue their treatment, as it may help lessen RLS symptoms by improving overall sleep quality.
Understanding the link between OSA and RLS is crucial for effective management and treatment. If you or someone you know experience symptoms like waking up gasping for air, loud snoring, or an uncontrollable urge to move your legs at night, consult a healthcare provider. Proper diagnosis and treatment can significantly improve your quality of life and prevent complications from these overlapping sleep disorders.
References
Gothi, Dipti, Rahul Kumar, Shweta Anand, Mahismita Patro, Nipun Malhotra, and Sameer Vaidya. “A Study on the Prevalence of RLS in Osa and the Consequences of Co-Occurrence.” U.S. National Library of Medicine, June 28, 2023.
Myc, Lukasz A., Ian T. Churnin, Mark J. Jameson, and Eric M. Davis. “Restless Leg Syndrome Is Common in Patients with Obstructive Sleep Apnoea | European Respiratory Society.” Journal of Clinical Sleep Medicine, October 15, 2018.
Pistorius, Franziska, Peter Geisler, Thomas C Wetter, and Tatjana Crönlein. “Sleep Apnea Syndrome Comorbid with and without Restless Legs Syndrome: Differences in Insomnia Specific Symptoms.” Sleep & breathing = Schlaf & Atmung, April 25, 2020.
“Restless Legs Syndrome.” Mayo Clinic, January 26, 2024.
Srakocic, S. “Restless Leg Syndrome and Sleep Apnea: What’s the Connection?” Healthline, May 24, 2024.
LEGAL DISCLAIMER: Material in this newsletter is provided for general health education and informational purposes and to provide references to other resources only; it may not apply to you as an individual. While Apria Healthcare believes that the information provided through this communication is accurate and reliable, Apria Healthcare cannot and does not make any such guarantee. It is not intended to be a replacement for professional medical advice, evaluation, diagnosis, services or treatment (collectively, “medical treatment”). Please see your healthcare provider for medical treatment related to you and your specific health condition(s). Never disregard medical advice or delay seeking medical care because of something you have read on or accessed through this website. Reading this newsletter should not be construed to mean that you have a healthcare provider/patient relationship.

.jpg?width=1120&height=376&name=AD-EmailBanner-TopSellingComfort_03.19.24%20(3).jpg)