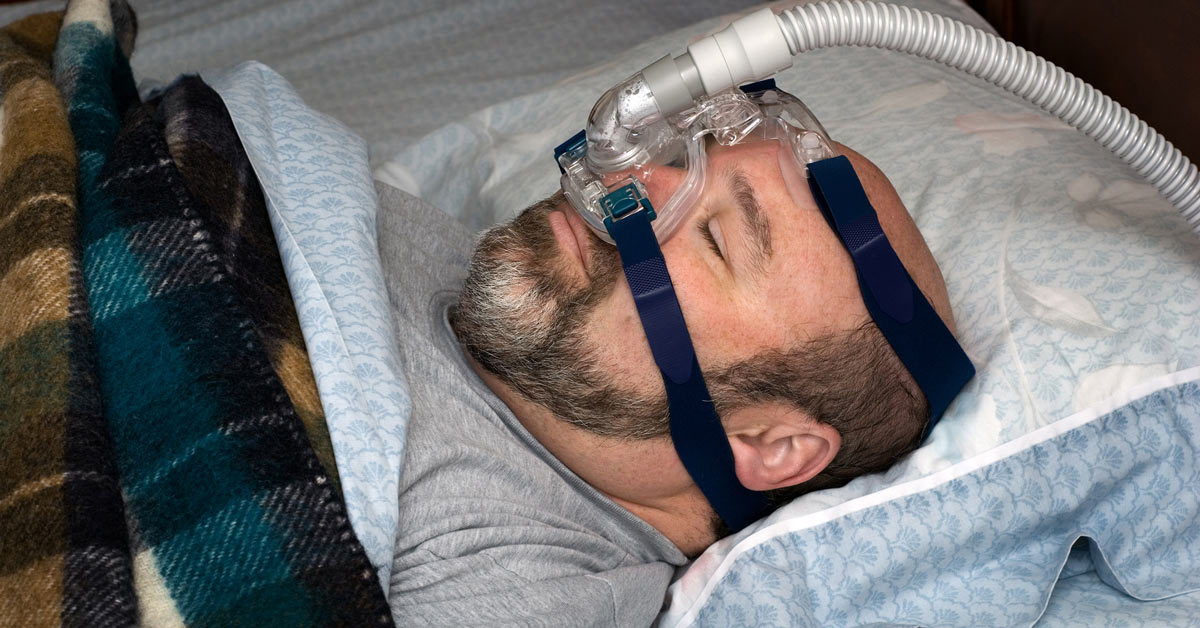
“Xerostomia” Affects Many People Who Use a CPAP Device to Treat Their Sleep Apnea. Here’s How to Stop It!
Chances are, you haven’t heard the word “xerostomia” (pronounced zeer-o-STOE-me-uh). It’s the medical term for the sensation of oral dryness, or dry mouth.
Xerostomia isn’t rare. In fact, up to 40% of people who use CPAP (continuous positive airway pressure) machines to treat their sleep apnea experience it.
For some people, dry mouth becomes so bothersome that they discontinue their CPAP therapy. But that can lead to even more severe health consequences, such as diabetes, heart disease, and obesity.
Robert Miller, Apria Healthcare Vice President of Sleep Business, states, “To ensure you continue with your CPAP therapy, it’s important for you to know about xerostomia—and how to prevent it.”
The Importance of Saliva
Dry mouth means you aren’t producing enough saliva. Saliva plays an important role in your health:
-
Aids in digestion
-
Reduces the growth of bacteria
-
Prevents tooth decay
-
Enhances your ability to taste
-
Helps remove food particles after eating
-
Simplifies chewing and swallowing
The Consequences of Dry Mouth
If your body isn’t producing enough saliva, you may experience the following:
- Sore throat and hoarseness
- Headaches and dizziness
- Increased tooth decay and gum disease
- Difficulty chewing and swallowing
- Thrush, which is a fungal infection of the mouth
- Bad breath
Apria’s Robert Miller adds, ”Xerostomia can also affect your sense of taste and enjoyment of food.”
Causes of Dry Mouth Beyond CPAP
CPAP therapy is not the only cause of dry mouth. Numerous factors may also contribute to this condition, including:
- Aging
- Cancer therapy
- Certain oral medications such as antihistamines and decongestants
- Nerve damage to your head and neck
- Problems with your salivary glands
- Health conditions such as diabetes, stroke, Alzheimer's disease, or HIV/AIDS
- Tobacco and alcohol use
- Recreational drug use, especially drugs like methamphetamine and marijuana
5 Ways to Prevent CPAP Dry Mouth
There are a variety of effective solutions to stop CPAP dry mouth. The best approach depends on its cause.
1. Keep the Air Moist
It’s important to keep the air you breathe moist.
A CPAP humidifier effectively replaces moisture by releasing warm, moist air from a small water chamber into the air delivered by your CPAP machine. (Note: This may cause CPAP “rainout,” a condition that can be easily resolved.)
Some CPAP machines have a humidifier built in. There are also external humidifiers that attach to your CPAP machine.
Inline heat moisture exchange (HME) humidifiers attach between the mask and tubing, and warm and moisten the air as you breathe.
Some CPAP machines use heated tubing to increase the moisture level and temperature of the pumped air, which may help with dry mouth.
You may also want to consider room humidifiers to help moisten the air in your bedroom and provide relief from xerostomia.
2. Make Sure Your CPAP Mask Fits
A mask that doesn’t fit properly and seal securely increases the risk of air leaks and dry mouth, which may reduce the effectiveness of your CPAP therapy. Research shows that 45% of people who stopped their CPAP therapy did so because of mask leaks.
That’s why it is important to work with your doctor to find the ideal mask for you. And refrain from overtightening it since this can lead to facial sores and marks on your face—and can be very uncomfortable.
3. Keep Your Mouth Closed When You Breathe
CPAP dry mouth is often caused by breathing through your mouth. So, if possible, breathe through your nose. If that doesn’t work, try a chin strap, which wraps around your head and chin to help keep your mouth closed.
Apria’s Robert Miller suggests, “If you use a nasal CPAP mask, ask your doctor about a full-face mask, which covers both your nose and mouth.”
4. Clear Nasal Congestion
Mouth breathing is often caused by nasal congestion. Your doctor may recommend saltwater sprays or oral medications that can clear nasal passages to help reduce mouth breathing.
Your doctor may conclude that your nasal congestion is caused by a deviated septum, which occurs when the thin wall separating your nasal passages is moved to one side. If so, a surgical procedure may be required.
5. Drink More Water
Your mouth may be dry because you are dehydrated. The solution: drink more water throughout the day. But not too close to bedtime since you don’t want to make multiple nighttime trips to the bathroom.
You Can Stop the Dry If You Try
CPAP dry mouth is annoying but also preventable. Simply follow the steps outlined above. If you continue to have xerostomia symptoms, make it a point to contact your doctor. Together, you can find a solution that will end your CPAP dry mouth so you can sleep comfortably again.
References
1. Dry mouth. Mayo Clinic. https://www.google.com/search?q=what+is+ xerostomia&oq=what+is+xerostomia&aqs=chrome..69i57j0i512l5j0i22i30l4.2780j0j7&sourceid=chrome&ie=UTF-8.
2. Common CPAP complaint: Dry mouth. ResMed. https://www.resmed.com/en-us/sleep-apnea/sleep-blog/common-cpap-complaint-dry-mouth/#:~:text=If%20you've%20ever%20felt,and%20difficulty%20talking%20or%20eating.
3. Summer, J. (Updated 2022, November 8). CPAP Dry Mouth: How to Stop It. Sleep Foundation. https://www.sleepfoundation.org/cpap/cpap-dry-mouth.
4. Peters, B. (Updated 2023, February 16). How to Prevent Dry Mouth During CPAP Therapy: Common Causes and Treatments. Verywell Health. https://www.verywellhealth.com/how-to-prevent-mouth-breathing-on-cpap-3015215.
5. Bond, L. (Updated 2023, February). Your Persistent Dry Mouth May Not Be CPAP Related. SleepApnea.Sleep-Disorders.net. https://sleepapnea.sleep-disorders.net/living/dry-mouth.
LEGAL DISCLAIMER: Material in this newsletter is provided for general health education and informational purposes and to provide references to other resources only; it may not apply to you as an individual. While Apria Healthcare believes that the information provided through this communication is accurate and reliable, Apria Healthcare cannot and does not make any such guarantee. It is not intended to be a replacement for professional medical advice, evaluation, diagnosis, services or treatment (collectively, “medical treatment”). Please see your healthcare provider for medical treatment related to you and your specific health condition(s). Never disregard medical advice or delay seeking medical care because of something you have read on or accessed through this website. Reading this newsletter should not be construed to mean that you have a healthcare provider/patient relationship.


.png)