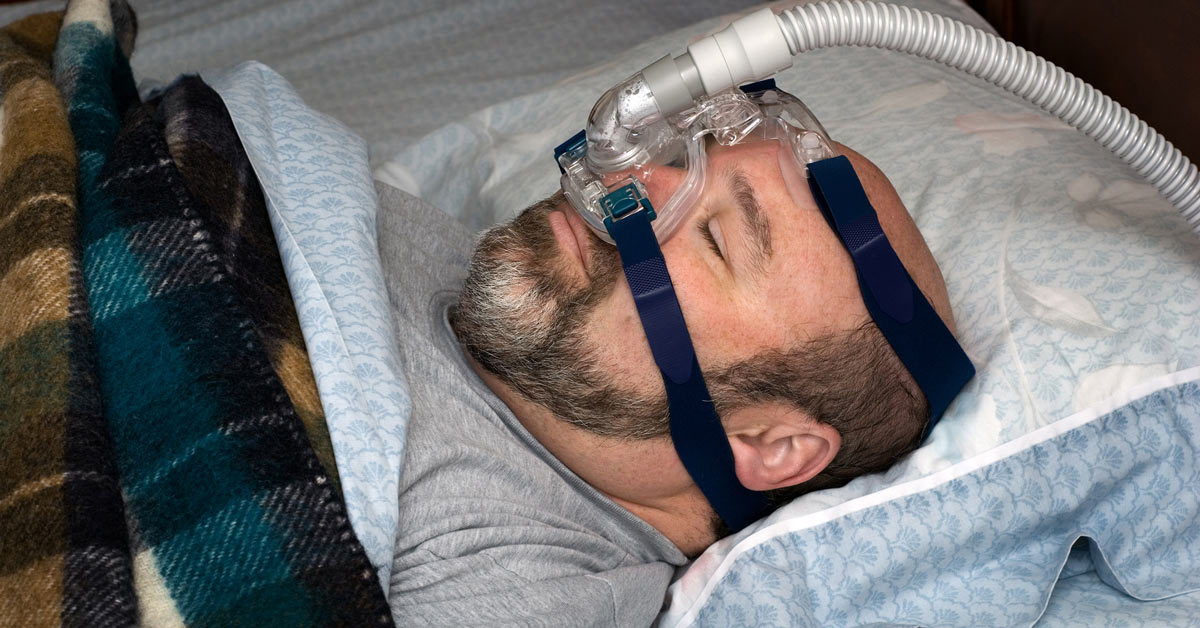
Your CPAP treatment doesn’t have to suffer.
It’s springtime! A time of year when many cheer the end of winter. For others, it signals the start of allergy season.
What triggers allergies (also known as allergic rhinitis and hay fever)? Allergens, which come in many forms, including dust mites, pollen, mold, and pet dander.
Allergens cause such symptoms as sneezing, coughing, itchiness, rashes, runny nose, watery eyes, and nasal congestion.
If you have sleep apnea, allergies can affect your sleep. Research reveals that sleep apnea symptoms can increase significantly in people with allergies.
And using a CPAP (continuous positive airway pressure) machine when you have allergies makes your therapy even more challenging.
Says Robert Miller, Apria Healthcare Vice President of Sleep Business, “Even during allergy season, you can get a good night’s sleep with your CPAP machine.”
How Allergies Affect Sleep Apnea
- Nasal congestion makes breathing difficult through a CPAP mask, especially if it covers your nose
- Sneezing and coughing can wake you throughout the night
- Allergic symptoms tend to worsen at night, leading to poor sleep quality
- Breathing through your nose adds moisture to your airways. Nasal congestion forces you to breathe through your mouth, drying out your throat and airways and making sleep uncomfortable
Some people may be tempted to stop their CPAP therapy because of allergies. But untreated sleep apnea can lead to some very serious health conditions, such as stroke and diabetes.
Here’s how to successfully continue your CPAP therapy—while reducing the amount of irritating allergens in your life.
1. Regularly Clean Your CPAP Machine
This helps keep it free of pollen, dust, and pathogens and reduces your risk of developing such conditions as pneumonia and sinus infections. Use warm water and mild soap to clean your mask, tubing, filters, and humidifier chamber.
2. Replace Your CPAP Supplies
The parts of a CPAP machine can break down and wear out over time. When that happens, cracks or scratches form, creating a home for bacteria. Be sure that your mask, tubing, and humidifier are in good working condition.
Replace your CPAP filters to prevent allergens from entering your airways while you sleep. Also, ask your doctor about hypoallergenic air filters, which trap even the tiniest particles.
3. Switch to a Full-face CPAP Mask
If you currently use a nasal CPAP mask, it’s probably more difficult to breathe through your nose when it is congested. Consider a full-face mask that covers both your nose and your mouth, which allows you to breathe through your mouth.
4. Humidify, Humidify, Humidify!
For some people, the pressurized air delivered by CPAP machines can reduce moisture in nasal passages. Plus, the congestion and inflammation caused by allergies can dry out your nose and throat.
A CPAP humidifier effectively replaces moisture by releasing warm, moist air from a small water chamber into the air delivered by your CPAP machine.
Some CPAP machines have a humidifier built in. There are also external humidifiers that attach to your CPAP machine.
5. Use the Ramp Feature on Your Machine
If you are having a hard time tolerating the continuous airflow delivered by your CPAP machine, the Ramp feature may help. It starts at a pressure so low that you barely notice it. Then it increases pressure to your prescribed pressure setting as you sleep. For many people, the Ramp feature helps them fall asleep more easily.
Most CPAP machines have this feature, but not all. But be sure to ask.
6. Consider Antihistamines
To drive allergens from your body, your immune system makes chemicals called histamines. But they can also cause sneezing and coughing, which make sleeping with your CPAP machine more difficult.
To combat these allergic reactions, your doctor may prescribe an antihistamine. Be sure to speak with your doctor before you begin any medication.
7. Keep Your Home, Bedroom, and Clothes Clean
Given the opportunity, allergens will make your home their home. That’s why it’s important to do a thorough house cleaning often. And keep your doors and windows closed during allergy season.
Your bedding is also a magnet for allergens, so change your sheets and pillowcases frequently.
Wash your clothes frequently too, especially if you are outdoors a lot. Use a dryer to dry clothes—don’t hang them outside to dry.
8. Shower Before Going to Bed
It’s a great way to wash away the allergens that have been collecting on your body and in your hair during the day. It will also help reduce the number of allergens in your bed.
9. Keep Pets Out of Your Bedroom
We know: they’re cute and you love them. (So do we.) But keeping pets out of your bedroom will reduce the allergen count. (You also may have more room in your bed to sleep!)
10. Talk to Your Doctor
Even though this tip appears last on this list, the first person you should call when you have questions about your condition or treatment is your doctor. Robert Miller states, “Your doctor will evaluate your allergies and how they are affecting your sleep and CPAP therapy then make the appropriate recommendations.”
The goal is to help improve the quality of your sleep and overall health—no matter what season it is.
References
1. Pacheco, D. (Updated 2022, April 1). Allergies and Sleep. Sleep Foundation. https://www.sleepfoundation.org/allergies-and-sleep.
2. Edwards, M. (Updated 2023, January 23). Allergies and Sleep. Sleep Apnea.org. https://www.sleepapnea.org/sleep-health/allergies-and-sleep/.
3. Lofta. (2023, March 23). Does Spring Mean Switching CPAP Styles?
Lofta. https://lofta.com/blogs/sleep-apnea/does-spring-mean-switching-cpap-styles.
4. CPAP and summer allergies. ResMed. https://www.resmed.com/en-us/sleep-apnea/sleep-blog/cpap-and-summer-allergies/.
5. Seasonal Allergies: Preparing Your CPAP for Fall. Lincare.
https://www.lincare.com/en/resources/blog/cpap-fall-allergies.
6. (2017, August 10). Are hay-fever or allergies affecting your CPAP use? ResMed. https://www.resmed.co.uk/patient/sleep-apnoea-blog/are-hay-fever-or-allergies-affecting-your-cpap-use/.
LEGAL DISCLAIMER: Material in this newsletter is provided for general health education and informational purposes and to provide references to other resources only; it may not apply to you as an individual. While Apria Healthcare believes that the information provided through this communication is accurate and reliable, Apria Healthcare cannot and does not make any such guarantee. It is not intended to be a replacement for professional medical advice, evaluation, diagnosis, services or treatment (collectively, “medical treatment”). Please see your healthcare provider for medical treatment related to you and your specific health condition(s). Never disregard medical advice or delay seeking medical care because of something you have read on or accessed through this website. Reading this newsletter should not be construed to mean that you have a healthcare provider/patient relationship.

.png)