It’s Called Nocturia, and It Can Disrupt Your Sleep
Research reveals that people with sleep apnea have higher rates of such urological conditions as erectile dysfunction, prostate cancer, and…nocturia?
You may be saying, “Nocturia? What’s that?”
It’s one of the more common conditions associated with sleep apnea.
Nocturia, also called nocturnal urination, is the frequent need to get out of bed and urinate throughout the night.
Apria Healthcare VP of Sleep Business Robert Miller states, “Although nocturia is relatively common—about 50 million Americans experience it—many people have never heard of it.”
For people with sleep apnea, it’s important to have a better understanding of nocturia and how it is treated.
Nocturia In a Nutshell
Everyone wakes up now and then in the middle of the night to go to the bathroom.
But if you are getting up two, three, four times or more per night, chances are you have nocturia.
Nocturia is not a disease but a symptom of other conditions such as sleep apnea.
Between the ages of 18 and 49, more women experience nocturia than men. Nocturia often happens during pregnancy but usually disappears about three months after giving birth.
After age 60, more men are affected. Nocturia is also more common among African-American and Hispanic adults.
Because nocturia involves urination, people often only tell their gynecologist or urologist about it, so it’s often attributed to prostate problems or aging.
Apria Robert Miller adds, “Many people don’t even mention it to their doctor—possibly because they are too embarrassed or think it is normal.”
What Nocturia Isn’t: Bedwetting
Nocturia causes you to wake up repeatedly to go to the bathroom. Wetting the bed is a different condition known as nocturnal enuresis or bedwetting.
Bedwetting is the involuntary release of urine as you sleep. It can be a symptom of bladder control problems like an overactive bladder or incontinence. It can also be caused by more serious conditions, such as an enlarged prostate or bladder cancer.
Risk Factors for Nocturia
In addition to sleep apnea, other factors are associated with nocturia:
- Diabetes
- Heart failure
- An enlarged prostate
- Bladder or urinary tract infection
- Problems with the veins in the lower legs
- Alcoholism
- Pregnancy
- Drinking fluids before bed
- Eating salty foods
- Taking certain medications
How Sleep Apnea Causes Nocturia
Studies show that about 50% of people with sleep apnea also have nocturia. There is even compelling evidence showing that sleep apnea may cause nocturia.
During an episode of sleep apnea, people experience a physiological chain reaction:
- The throat’s soft structures relax, which blocks airways
- Oxygen levels decrease and carbon dioxide levels increase
- Your blood becomes more acidic, your heart rate drops, and your lungs’ blood vessels constrict
- To reopen the airways, you wake up
- Because your heart is racing and receiving false signals of fluid overload, your heart excretes a protein that helps rid the body of excess sodium and water
The result: nocturia.
The Consequences of Nocturia
Making multiple bathroom trips during the night disrupts your sleep and makes it difficult to fall asleep when you crawl back into bed. This can result in:
- Excessive daytime sleepiness
- Higher risk of falls and fractures
- Depression
- Irritability
- Impaired mental and physical function
If left untreated, nocturia can negatively affect your overall health and well-being.
Treating Sleep Apnea Also Helps Treat Nocturia
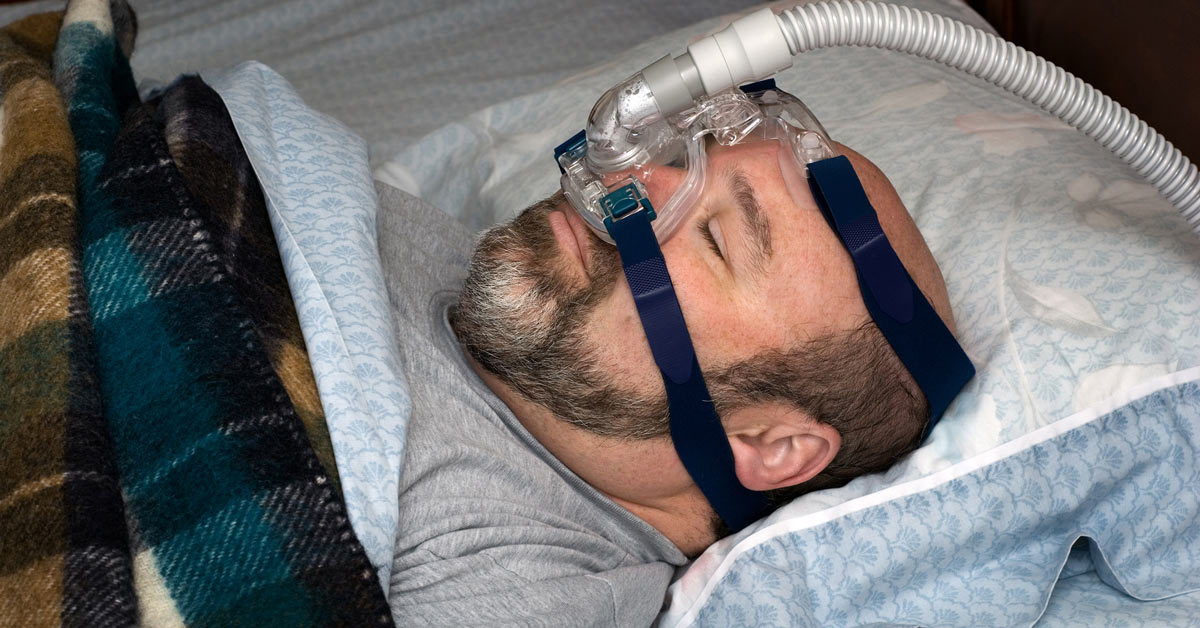
A proven method of effectively treating sleep apnea is with a CPAP (continuous positive air pressure) machine. In fact, more than 8 million Americans use CPAP machines to treat their condition. That’s why CPAP is considered the “gold standard” of sleep apnea care.
CPAP involves wearing a mask that fits comfortably over your nose or mouth while you sleep. The mask is connected to a machine by your bed that provides a constant, quiet flow of air to keep your airways open so you can breathe—and sleep—normally.
Apria’s Robert Miller adds, “Numerous studies report significant reductions in the number of nocturia incidents with people who use their CPAP machine.”
In addition to CPAP, there are also lifestyle changes you can make to reduce the number of nighttime bathroom breaks:
- Reduce the amount of fluid you drink before bedtime
- Eat fewer salty foods and snacks
- Practice proper sleep hygiene: maintain a regular sleep/wake routine, ensure your bedroom is dark, cool, and comfortable, and learn relaxation techniques
- Decrease your consumption of caffeine and alcohol, especially in the afternoon and evening
- Limit the use of electronic devices before bedtime
- Speak with your doctor about possible medications to treat nocturia
Don’t Lose Sleep Over Nocturia
Although nocturia is common, it is very treatable. If you find you are repeatedly making multiple trips to the bathroom during the night, speak with your doctor. Together, you can make a plan to help improve the quality and quantity of sleep so you can start each day rested and refreshed.
References
1. Chung SD, et al. Obstructive sleep apnea and urological comorbidities in males: a population-based study. Sleep and Breath. 2016 Dec;20(4):1203-1208.
2. Suni, E. (Updated 2022, October 7). Nocturia or Frequent Urination at Night. Sleep Foundation. https://www.sleepfoundation.org/physical-health/nocturia-or-frequent-unrination-night.
3. Doyle-McClam M, et al. Nocturia in Women With Obstructive Sleep Apnea.
Am J Lifestyle Med. 2021 May-Jun;15(3):260–268.
4. Ikpeze, T. (Updated 2022, October 28). Nighttime Urination & Sleep Apnea. SleepApnea.org. https://www.sleepapnea.org/sleep-health/nighttime-urination-and-sleep-apnea/.
5. Preidt, R. (2017, March 27). Treating Sleep Apnea May Ease Night Bathroom Trips. WebMD. https://www.webmd.com/sleep-disorders/sleep-apnea/news/20170327/curbing-sleep-apnea-might-mean-fewer-night-trips-to-bathroom.
6. (2000, April 27). Study Links Sleep Disorder and Nighttime Urinating. The University of Alabama at Birmingham. https://www.uab.edu/newsarchive/43392-study-links-sleep-disorder-and-nighttime-urinating.
LEGAL DISCLAIMER: Material in this newsletter is provided for general health education and informational purposes and to provide references to other resources only; it may not apply to you as an individual. While Apria Healthcare believes that the information provided through this communication is accurate and reliable, Apria Healthcare cannot and does not make any such guarantee. It is not intended to be a replacement for professional medical advice, evaluation, diagnosis, services or treatment (collectively, “medical treatment”). Please see your healthcare provider for medical treatment related to you and your specific health condition(s). Never disregard medical advice or delay seeking medical care because of something you have read on or accessed through this website. Reading this newsletter should not be construed to mean that you have a healthcare provider/patient relationship.

.png)